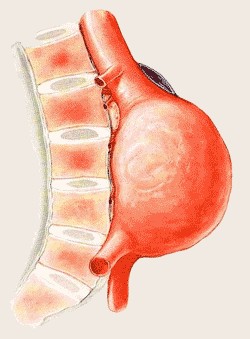
Abdominal Aortic Aneurysm
(not good…!!!)
The last couple of weeks have been something of a blur. This usually happens after my night shifts.
Did another tour of duty on the Foxtrot-Oscar Paramedic/Police unit which lo and behold involved lots of lovely assaults and drink related injuries. Nice! But it still works well when we we can treat on scene and point the customer in the direction of A/E if its only a minor injury.
I seem to be getting to know all the regular places and can pin-point the likely time and location of our first job in a “Crocodile Dundee” sort of way.
The vast majority of jobs on the truck have been pretty run of the mill stuff. I say run of the mill as I can run a “chest pains” call with my eyes shut I think. (I wont just in case I treat the wrong patient!) Others have included TIAs (Transient Ischaemic Attacks…basically mini strokes), CVAs (Cerebro Vascular Accidents…basically proper full blown strokes) SOBs (basically Shortness of Breath…due to asthma, bronchitis etc) and PITAs (basically “Pain In The Arse” jobs…life is too short to explain in depth)
But every now and then a job pops up on the old “earn your money” radar. And last week the radar spotted us under our cloak of stealth and invisibility.
We were called on three 9s to attend a gent in his mid sixties with abdo pain. So off we went on “blues & twos” to the address expecting to find someone with “tummy ache” or “Deli belly” or a “bit off” or with an attack of the “squits”.
We pulled up outside the address having made good time and took the resus bag inside (no matter what job I go to I always take the bag as you never know and I have been caught out before as I,m sure many others have in the service).
Inside we found our patient who appeared well on first sight. The first thing he, and his wife said was “You,ve just missed the doctor…he left not more than a minute or so ago.”
Having not been told by “Puzzle Palace” (Command & Control) that a GP was on scene we asked the next relevant question…”Has the GP left a letter (usually a scribbled note to the receiving hospital about the patients presenting complaint, medical history and any observations with a provisional diagnosis) These letters help us to speed things up as it gives us good information (sometimes) and a set of baseline obs (occasionally) to be going on with.
“No…he did,nt leave a letter.”
“Okay…did he tell you what might be wrong with you?”
“No…he just made a phone call and said that I should go to hospital.”
“Okay…did the doctor examine you?”
“Erm…kind of…he just pushed on my belly and that was it.”
Great…another job where the GP has dialled 999 because he thinks this chap should be in hospital and then he,s gone and buggered off! Thanks!
So we have to start from the beginning…presenting complaint=2-3 day history of abdo pain, gradual onset although today the pain has intensified. He has vomited once today and has not eaten for two whole days. We know the chaps GCS is 15/15 obviously cos hes talking to us and breathing at the same time…marvellous thing is nature.
Checking his obs we find he has a pulse of around 110 with a Blood Pressure of approx 120/68. He looks pale and feels “dizzy” when he stands. His 02 saturation levels are 78% on air and 84% on oxygen. I have a quick look at the chaps abdomen looking for anything obvious…seems okay. I then have a feel around his abdo to see where the pain is concentrated or where it radiates to….just beneath his naval around the umbilicus area (obviously) I place my hands and find….”boom boom boom boom boom boom boom”.
“Ahhhh….(bugger)”.
I feel his heart beat, his pulse, his life blood pumping away like a steam train. I found it strange that I could not see any pulsating mass using the “number 1 mark 1 eyeball”.
The chap was in some degree of pain, although it was bearable. I knew we had to sort him on the truck and foxtrot-oscar to the hospital sharpish. Within a couple of minutes he was on the stretcher, on oxygen, being monitored and an alert call was put in for resus to stand by. A line was put in en-route as a KVO. (Keep Vein Open)
All this took less than ten minutes whilst at the same time putting the chaps mind at rest. If one of these things burst outside of hospital (or specifically an operating theatre) the mortality rate is in the high 90s!
He was in the operating theatre within 30 minutes of our arrival at resus…………………………………
———————————————–
What are the symptoms?
Many people do not feel any symptoms with an abdominal aortic aneurysm. Occasionally, patients can experience:
- A pulsing feeling in the abdomen, similar to a heartbeat.
- Severe, sudden pain in your abdomen or lower back. If this is the case, your aneurysm may be about to rupture.
If your aneurysm ruptures, you may suddenly feel intense weakness, dizziness, or back pain, and you may lose consciousness. This is a life- threatening situation and you should seek medical attention immediately.
What causes an abdominal aortic aneurysm?
The etiology of an aneurysm is probably multi-factorial. The leading thought is that the aneurysm may be caused by inflammation in the aorta, which may cause its wall to break down. Some researches believe that this inflammation can be associated with atherosclerosis (also called hardening of the arteries) and risk factors that contribute to atherosclerosis, such as high blood pressure (hypertension).
———————————————–
I saw him a few days ago on the recovery ward. He had suffered an 11 cm AAA. In terms of AAAs this was a massive one and he was lucky to survive it. (The survival rate in surgery is around 50%!)
It was a good feeling to see him looking well and he told me that he did,nt realise how poorly he was until the surgeon told him his chances of survival.
He was happy…and so was I. It makes up for all the crap jobs we get….a bit!




 Posted by kingmagic
Posted by kingmagic 



